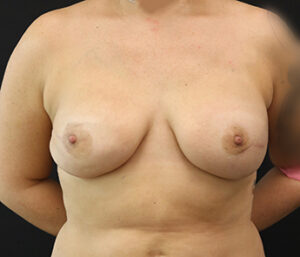
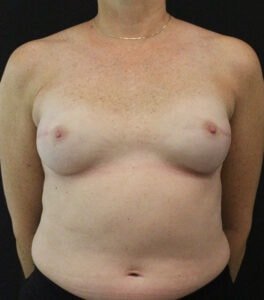
Breast Reconstruction
Breast Reconstruction can be an exceptionally rewarding and empowering option for women who receive a mastectomy as part of their battle to beat breast cancer. Several different techniques can be employed to rebuild the breast mound following mastectomy, each of which can help restore a normal shape, size, and overall appearance to the breast(s). At our practice, board-certified plastic surgeon Stafford Broumand, M.D. offers implant reconstruction, fat grafting, and DIEP flap breast reconstruction. He will work closely with you to customize an approach that most effectively achieves an ideal outcome based on your unique needs and desires.
What Is Breast Reconstruction?
Breast reconstruction encompasses a series of surgical procedures designed to recreate a breast that has been removed or altered due to
Trusted Source
Breast Reconstruction
ASPS
Go to Source
cancer treatment
or other diseases. The goal is to rebuild the breast to near-normal shape, size, and appearance. This can involve placing implants, autologous tissue (using the patient’s own tissue from another part of the body), or a combination of both. Techniques and timing (immediate vs. delayed reconstruction) are tailored to fit the individual’s specific circumstances, considering factors such as the type of cancer treatment received and personal preferences.

Benefits of Breast Reconstruction
The benefits of undergoing breast reconstruction are multifaceted, including:
- Restoration of Body Symmetry: Helps in achieving a balanced look, especially important for those who have had a single mastectomy.
- Enhancement of Self-Image: Plays a crucial role in improving psychological well-being and confidence after breast loss.
- Elimination of the Need for External Prostheses: Provides a permanent solution that can eliminate the discomfort and inconvenience associated with external breast forms.
- Customizable Results: Offers various reconstructive options to meet individual needs and preferences, allowing for personalization in achieving desired outcomes.
Candidates for Breast Reconstruction
Ideal candidates for breast reconstruction are those who have undergone mastectomy or lumpectomy or have experienced breast deformity due to congenital defects, trauma, or other conditions. It is suitable for individuals looking to restore breast appearance for personal or aesthetic reasons. Candidates should be in good overall health, have a positive outlook with realistic expectations, and be nonsmokers or willing to quit, as smoking can impede the healing process.

Preparing for Breast Reconstruction
Preparation for breast reconstruction involves an in-depth consultation with Dr. Broumand. During this consultation, he will assess your health, discuss your reconstructive options including the placement of incisions, and develop a personalized treatment plan. Preparation may also involve getting baseline mammograms, adjusting current medications, and, if you smoke, taking steps to stop. Ensuring you have a support system in place for post-operative care and recovery is crucial.
The Breast Reconstruction Procedure
Breast reconstruction techniques vary widely and may include the use of breast implants, flap reconstruction (using the patient’s own tissue), or a combination of both. The choice of technique depends on several factors, including the patient’s body type, medical history, and desired outcome. Reconstructive breast surgery procedures can be performed immediately following mastectomy or delayed until after the patient has recovered from mastectomy and completed any additional cancer treatments. Dr. Broumand is proud to offer the following breast reconstruction procedures:
Breast Implant Reconstruction
Implant-based reconstruction is a technique that involves the placement of silicone or saline implants to recreate the breast mound after mastectomy, similar to breast augmentation. This process can be done in stages, starting with the insertion of a tissue expander to stretch the skin and make room for the breast implant. Once the tissue expansion is adequate, the expander is replaced with a permanent implant during subsequent surgery. This method is often chosen for its shorter initial recovery time and because it does not require tissue to be taken from other parts of the body, making it a less invasive option for breast reconstruction.
Breast Reconstruction with Fat Grafting
Breast reconstruction with fat grafting, also known as autologous fat transfer, involves using the patient’s own fat cells to reconstruct the breast. Fat is harvested from other areas of the body, such as the abdomen, thighs, or buttocks, through liposuction. The fat is then processed and injected into the breast area to create a natural-looking breast shape. This technique can be used on its own for smaller volume enhancements or in conjunction with other reconstruction methods to refine the shape and feel of the reconstructed breast. It is particularly valued for its ability to achieve more natural results and for the dual benefit of contouring the area from which the fat is taken.
DIEP Flap Breast Reconstruction
DIEP flap (Deep Inferior Epigastric Perforator flap) breast reconstruction is a sophisticated procedure that uses the patient’s own
Trusted Source
Breast reconstruction with flap surgery
Mayo Clinic
Go to Source
abdominal skin
and fat to reconstruct the breast, without sacrificing the abdominal muscles. The DIEP flap is carefully dissected from the original blood supply on the abdomen and transferred to the chest, where it is shaped into a new breast mound and connected to the chest blood vessels using microsurgery. This technique is favored for its ability to create a breast that looks and feels like natural breasts, while also offering the added benefit of a flatter abdomen, much like a tummy tuck. It is considered a more complex and time-consuming procedure but is highly regarded for its aesthetic outcomes and muscle-preserving approach.
Nipple-Sparing Mastectomy
In certain cases, a nipple-sparing mastectomy—which only removes the underlying breast tissue—can be conducted before these Breast Reconstruction techniques to help maintain more of your own anatomy through the preservation of breast skin and the nipple-areola complex. Additionally, the resulting scar may be better concealed in comparison to that of a standard mastectomy and nipple reconstruction operation. Whether or not this advanced mastectomy approach may be right for you can be discussed in full detail at the time of your consultation with Dr. Broumand.


Breast Reconstruction Recovery & Results
The recovery process following breast reconstruction varies depending on the type of surgery performed. Initial recovery typically involves a hospital stay, followed by several weeks of rest and limited activity at home. Your breast reconstruction surgeon, Dr. Broumand, will provide detailed post-operative care instructions and schedule follow-up appointments to monitor your healing. The final results of breast reconstruction gradually develop over time as swelling decreases and the breast shape stabilizes, offering a renewed sense of wholeness and femininity.
How long does breast reconstruction surgery take?
The duration of breast reconstruction surgery varies based on the technique used and whether one or both breasts are being reconstructed. It can range from 1 to 6 hours.
Will there be visible scars after breast reconstruction?
Scarring is inevitable following breast reconstruction, but Dr. Broumand employs techniques to minimize their appearance. Scars typically fade over time but will not disappear completely.
How long is the recovery period after breast reconstruction?
Recovery can vary, with initial downtime ranging from 6 to 8 weeks. Full recovery and the final results can take several months to a year, especially if multiple procedures are involved.
When can I return to normal activities after breast reconstruction?
Most patients can resume light activities within 4 to 6 weeks post-surgery. Strenuous activities and heavy lifting should be avoided for at least 6 to 8 weeks.
Are the results of breast reconstruction permanent?
While the results of breast reconstruction are long-lasting, factors such as weight fluctuations, aging, and hormonal changes can affect the appearance of the reconstructed breast over time.
What are the risks associated with breast reconstruction?
Risks include infection, bleeding, flap failure, complications with implants, and changes in breast or
Trusted Source
What to Expect After Breast Reconstruction Surgery
American Cancer Society
Go to Source
nipple sensation
, among others. Dr. Broumand will discuss these in detail during your consultation.
Can I combine a breast lift with breast reconstruction?
Yes, combining a breast lift with breast reconstruction is a common and feasible approach for many patients. This combination allows for the restoration of breast volume and shape following mastectomy or lumpectomy, while also addressing sagging to achieve a more youthful and uplifted breast profile. The breast lift (mastopexy) can enhance the overall appearance of the reconstructed breast, ensuring symmetry and improving contour. This integrated approach is tailored to each patient’s specific needs and desired outcomes, and it is best to discuss your options and expectations with Dr. Broumand, who can provide personalized advice based on your unique situation.
Is breast reconstruction covered by insurance?
In many cases, this type of reconstructive plastic surgery is
Trusted Source
Women's Health and Cancer Rights Act (WHCRA)
Centers for Medicare and Medicaid Services
Go to Source
covered by insurance
under the Women’s Health and Cancer Rights Act. Dr. Broumand’s team can assist with navigating coverage with your insurance company.
Schedule A Consultation For Breast Reconstruction
If you are considering breast reconstruction in Manhattan, Dr. Stafford Broumand brings extensive experience and a compassionate approach to help you through your reconstructive journey. Contact us at our Park Avenue practice in New York City today to schedule your consultation today to explore your breast reconstruction options and embark on a path toward physical and emotional healing.

Contact Us
1 ASPS. Breast Reconstruction. Available: https://www.plasticsurgery.org/reconstructive-procedures/breast-reconstruction. Accessed February 13, 2024.
2 Mayo Clinic. Breast reconstruction with flap surgery. Available: https://www.mayoclinic.org/tests-procedures/breast-reconstruction-flap/about/pac-20384937. Accessed February 13, 2024.
3 American Cancer Society. What to Expect After Breast Reconstruction Surgery. Available: https://www.cancer.org/cancer/types/breast-cancer/reconstruction-surgery/what-to-expect-after-breast-reconstruction-surgery.html. Accessed February 13, 2024.
4 Centers for Medicare and Medicaid Services. Women’s Health and Cancer Rights Act (WHCRA). Available: https://www.cms.gov/cciio/programs-and-initiatives/other-insurance-protections/whcra_factsheet#. Accessed February 13, 2024.
Dr. Stafford Broumand has reviewed and approved this content.
Page Updated: